Unusual complications related to guidewire use during ERCP: an unappreciated injuries
Fouad Nejjari, Salma Ouahid, Tarik Adioui, Sanaa Berrag, Tarik Addajou, Mouna Tamzaourte, Aziz Aourarh
Corresponding author: Fouad Nejjari, Gastroenterology Unit, 5th Military Hospital, Guelmim, Morocco 
Received: 07 Nov 2019 - Accepted: 15 Nov 2019 - Published: 18 Nov 2019
Domain: Gastroenterology,Hepatology
Keywords: ERCP, guidewire, complications, subcapsular hematoma, stripping
©Fouad Nejjari et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Fouad Nejjari et al. Unusual complications related to guidewire use during ERCP: an unappreciated injuries. PAMJ Clinical Medicine. 2019;1:15. [doi: 10.11604/pamj-cm.2019.1.15.20913]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/1/15/full
Unusual complications related to guidewire use during ERCP: an unappreciated injuries
Fouad Nejjari1,&, Salma Ouahid2, Tarik Adioui1, Sanaa Berrag2, Tarik Addajou2, Mouna Tamzaourte2, Aziz Aourarh2
1Gastroenterology Unit, 5th Military Hospital, Guelmim, Morocco, 2Gastroenterology I Unit, Mohamed V Military Teaching Hospital, Rabat, Morocco
&Corresponding author
Fouad Nejjari, Gastroenterology Unit, 5th Military Hospital, Guelmim, Morocco
Endoscopic retrograde cholangiopancreatography is an endoscopic procedure with relatively low complication risk. The most frequent complications are pancreatitis, cholangitis, hemorrage and perforation. Other complications specific to guidewire use reported in literature include duodenal perforation, liver and pancreatic parenchyma perforation, and guidewire fracture. We report a case of hepatic subcapsular hematoma and a case of stripped and fractured guidewire during ERCP, which were successfully managed with nonsurgical approach. These cases illustrate examples of unusual but serious complications related to guidewire use during ERCP.
Endoscopic retrograde cholangiopancreatography (ERCP) is an indispensable tool for management of various pancreaticobiliary disorders. Pancreatitis, cholangitis, perforation and bleeding have been the most frequently described complications. Infrequent complications specific to the guidewire use described in the literature include: duodenal perforation, liver and pancreatic parenchyma perforation, and guidewire fracture. We report a case of subcapsulair hepatic hematoma and a case of stripping and fracture of guidewire during ERCP, which were successfully managed with conservative approach.
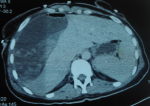
Case 1: a 39-year-old woman with history of acute pancreatitis presented with fluctuating jaundice, right upper quadrant pain, and intermittent vomiting. Physical examination revealed little upper abdominal quadrant tenderness. Biochemistry demonstrated hepatic cytolysis and cholestasis. Ultrasound and magnetic resonance imaging showed dilated common-bile-duct above multiple stones. ERCP was performed and cholangiopancreatography reveled a marked dilation of common-bile-duct (CBD) with multiple large calculi which were successfully extracted after endoscopic sphincterotomy. Six hours after procedure, the patient complained of intense upper right quadrant abdominal pain with tenderness. Lipase and haemoglobin were within normal ranges. Urgent computed tomography (CT) showed a large right Subcapsular hepatic hematoma (8-16 cm) with air bubbles within the collection (Figure 1). The patient was treated conservatively with analgesia, intravenous antibiotics, and blood transfusion, and closely monitored. Haemoglobin remained stable, but the c-reactive-protein (CRP) raised to 300 mg/l and procalcitonine to 3 ug/L. Thus, percutaneous drainage was performed and 1000 ml of bloody fluid was removed. During follow up, abdominal CT showed marked reduction of hematoma with no further complications.
�
Case 2: a 31 year-old-man with a recent history of diabetes was admitted for abdominal pain and vomiting. Abdominal computed tomography suggested chronic pancreatitis with dilated main pancreatic duct (MPD) and multiples calcifications. Endoscopic retrograde cholangiopancreatography revealed an irregular and dilated MPD with multiple calculi, after pancreatic sphincterotomy, a guidewire was introduced into the MPD but was incrusted around pancreatic calculi, attempts to remove the guidewire led to stripping and fragmentation leaving a short wire fragment in the MPD. The patient had no acute complications, an Abdomen CT realised two months after ERCP reveled no complication related to the retained wire fragment, and the patient remains asymptomatic one year after the guidewire fragmentation.
Post-ERCP hepatic Subcapsular hematoma is a rare complication. The first case was reported in 2000 by Ortega [1]. Only few cases were described in literature afterwards. This complication may be misdiagnosed while morphologic post-ERCP monitoring is not routinely performed [2]. The pathogenesis is not clear, proposed mechanisms are accidental puncture with laceration and rupture of small intrahepatic vessels and bile ductules, or capsule perforation by the guide-wire [2] this also explain the existence of air inside the hematoma and frequent infection due to the use of a guide-wire with a non sterile technique [3]. Another mechanism is the rupture of bile ductules and vessels secondary to the force exerted with the balloon when trying to remove a retained calculus [4]. Clinical manifestations include abdominal pain, syncope, hemodynamic instability, anaemia and fever. After ERCP, patient with symptoms should underwent morphologic assessment (ultrasound, CT) to confirm and monitor this emergent complication [3,5]. 29 cases were reported to date, 12 patients (41%) were treated conservatively using analgesia, antibiotics, intravenous fluids, blood transfusion and octreotide, 8 patients (27%) with percutaneous drainage, 6 patients (20%) with embolization and 3 patients (10%) required surgical management [5-7].The outcome was often favourable except for one case of fatal hematoma rupture [8,9] Guidewire fracture during ERCP is an uncommon event. The proposed mechanisms includes: forceful traction, excessive rotational forces, and imperfection of the floppy coating with potential electrical short circuit. The theoretical risks of retained guidewire fragment include: infection or abscess formation, recently a case of migration of the fractured guidewire was described [10]. Very few cases of fractured guidewire in main pancreatic duct have been described and often the fractured guidewire appears to be irretrievable by endoscopy, left in situ in asymptomatic patients. Wipple's intervention was necessary in other symptomatic patients [10].
Complications related to guidewire use during ERCP are rare but potentially serious and must be known for early detection, diagnosis and management, to minimize their morbidity and mortality.
The author declare no competing interests
All the authors have read and agreed to the final manuscript.
Figure 1: computed tomography (CT) image showing large subcapsular hepatic hematoma (8-16 cm) in maximum dimentions with air inside, following (ERCP)
- Ortega Deballon P, Fern�ndez Lobato R, Garc�a Septiem J, Nieves V�zquez MA, Mart�nez Santos C, Moreno Azcoita M. Liver hematoma following endoscopic retrograde cholangiopancreatography (ERCP). Surg Endosc. 2000;14(8):767. PubMed | Google Scholar
- Orellana F, Irarrazaval J, Galindo J, Balbontin P, Manr�quez L, Plass R et al. Subcapsular hepatic hematoma post ERCP: a rare or an underdiagnosed complication. Endoscopy. 2012;44 Suppl 2 UCTN:E108-109. PubMed | Google Scholar
- Chi KD, Waxman I. Subcapsular Hepatic Hematoma after guide wire injury during endoscopic retrograde cholangiopancreatography: management and review. Endoscopy. 2004;36(11):1019-1021. PubMed | Google Scholar
- Baudet J-S, Argui�arena X, Redondo I, Tadeo E, Navazo L, Mendiz J et al. Hematoma hep�tico subcapsular. Una rara complicaci�n de la CPRE. Gastroenterol Hepatol. 2011;34(2):79-82. Google Scholar
- del Moral Mart�nez M, Delgado Maroto A, Cervilla S�ez de Tejada ME, Casado Caballero FJ, Salmer�n Escobar FJ. Hepatic hematoma after ERCP: two new case reports. Rev Esp Enfermedades Dig. 2017 Jun;109(6):470-473. PubMed | Google Scholar
- Zappa MA, Aiolfi A, Antonini I, Musolino CD, Porta A. Subcapsular hepatic haematoma of the right lobe following endoscopic retrograde cholangiopancreatography: case report and literature review. World J Gastroenterol. 2016;22(17):4411. PubMed | Google Scholar
- Soler Humanes R, Su�rez Mu�oz M�, Garc�a Garc�a B. A post-endoscopic retrograde cholangiopancreatography subcapsular hepatic hematoma. Rev Esp Enfermedades Dig. 2017;109(11):803. Google Scholar
- Gonz�lez-L�pez R, Garc�a-Cano E, Espinosa-Gonz�lez O, Cruz-Salgado �, Montiel-Jarquin �-J, Hern�ndez-Zamora V. Tratamiento quir�rgico para hematoma subcapsular hep�tico posterior a colangiograf�a retr�grada endosc�pica; caso inusual. Cir Cir. 2015;83(6):506�509. Google Scholar
- Kl�mov� K, Su�rez CP, Asanza CG, Pe�a AM, Arregui EC, Alonso AH. Subcapsular hepatic hematoma after ERCP: a case report and revision of literature. Case Rep Clin Med. 2014;03(03):161-166. Google Scholar
- Pruitt A, Schutz SM, Baron T, McClendon D, Lang KA. Fractured hydrophilic guidewire during ERCP: a case series. Gastrointest Endosc. 1998;48(1):77-80. PubMed | Google Scholar